Zero balance review software is a specialized type of revenue cycle technology that automatically audits patient accounts marked "paid in full" or otherwise closed, looking for underpayments, denial errors, and contractual variances that slipped past front-line collection processes. Because the account already shows a zero balance, these missed dollars sit invisible on financial reports - yet they often represent 1% to 3% of net patient revenue, and sometimes more.
This guide explains what zero balance review software does, how it works, what features matter, and how to evaluate options for your organization.
What is zero balance review software?
Zero balance review software is a platform that retrospectively analyzes accounts with no remaining balance to verify whether the provider was paid the full contractual amount. The software ingests payer remittance data, billed charges, and contracted reimbursement terms, then flags any account where the actual payment fell short of the expected amount - even after the account has been closed.
In practical terms, it acts as a safety net behind the primary AR workflow. Standard accounts receivable tools focus on open balances. Zero balance review software focuses on the accounts everyone else has stopped looking at.
Why zero balance review matters
Closed accounts hide more revenue than most providers realize. According to a Becker's Hospital Review study summarized by MD Clarity, providers lose 1% to 3% of net revenue annually to payer underpayments. AGS Health research puts the share of underpaid claims at 7% to 11%. And according to the American Hospital Association, hospitals absorbed $130 billion in Medicare and Medicaid underpayments in 2023 alone.

The reason these losses persist is structural. Payers rarely send a notification saying "we short-paid you by $18 because we grouped your code incorrectly." Instead, a partial payment posts, the contractual adjustment swallows the rest, and the account closes. Without dedicated software comparing every line item to contract terms, those variances remain invisible.
A few examples of what hides inside a zero balance account:
- Payments below the contracted CPT-level rate
- Denied line items written off rather than appealed
- Bundled or downcoded services missing payment
- Sequestration, modifier, or multiple-procedure reductions applied incorrectly
- Patient responsibility miscalculated or misposted
Manual zero balance review is no longer viable
Some organizations still audit closed accounts manually with spreadsheets. The math does not work. Payment variance research found the average underpayment is roughly $38 per line item - small enough to feel like noise, but a midsized group submitting 20,000 claims a month at a 2.5% underpayment rate sheds hundreds of thousands of dollars per year.
Manual review also struggles with modern payer contract complexity. Reimbursement formulas now layer GPCI adjustments, lesser-of clauses, modifier rules, bundling logic, mid-level differentials, and percent-of-charge methodologies. A spreadsheet cannot reliably calculate the expected reimbursement for every claim, much less do it across hundreds of millions of claims per month. Software is the only practical path.
Core features of zero balance review software
Not all platforms are built the same. The most effective zero balance review software shares a common feature set.
Contract digitization and a centralized repository
The software ingests payer contracts in whatever format they exist - PDFs, spreadsheets, emails - and converts them into a single, version-controlled library of rate tables and terms. Without this layer, the engine has nothing to compare payments against.
Charge-level variance detection
Strong platforms compare every remittance to the contracted rate at the CPT, HCPCS, modifier, and site-of-service level - not at the claim header level. Header-level comparisons miss variances buried inside complex multi-line claims.
Full simulation of payer adjudication logic
The detection engine should model how each payer actually adjudicates a claim, including GPCI and locality adjustments, multiple-procedure reductions, lesser-of clauses, sequestration, modifier rules, bundling, packaging, mid-level differentials, and patient responsibility. Comparing claim totals to a flat fee schedule misses most of the real variance.
Automated worklist routing
When a variance is detected, the software should automatically assign the account to the right staff worklist with the contract language and ERA detail attached, so the team can pursue recovery without rebuilding the analysis from scratch.
Root cause analytics
Detection only solves half the problem. Reporting should surface patterns by payer, contract, CPT code, location, and physician so leaders can fix the upstream drivers, whether those are payer behavior, contract language, or internal coding issues.
Contract modeling
Mature platforms let revenue cycle leaders model the net revenue impact of proposed contract changes before negotiating, so negotiations are anchored in data rather than instinct.
How zero balance review software works
The workflow is straightforward once contracts and data are loaded.
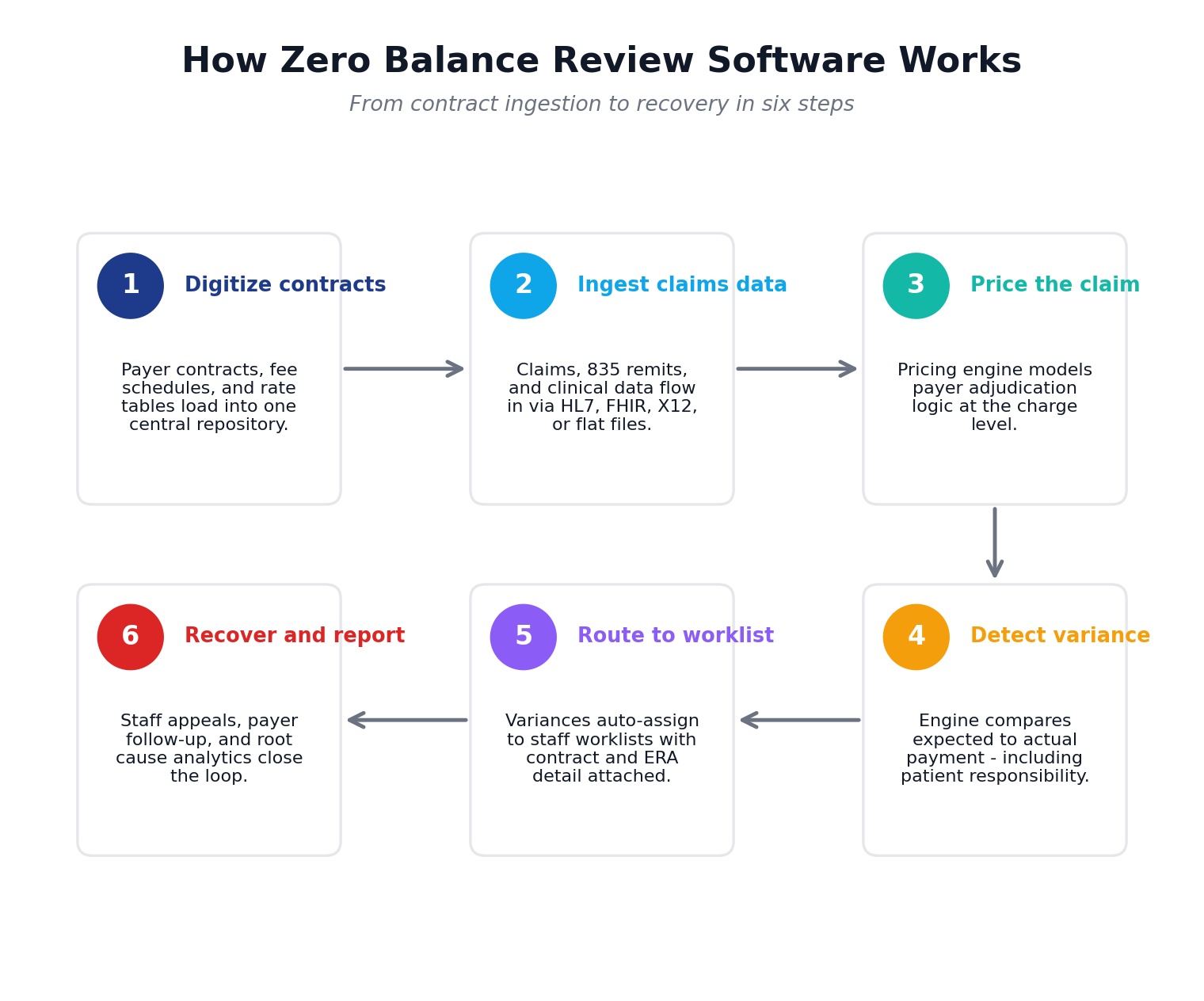
- Contracts digitized. Payer contracts and fee schedules load into a central repository.
- Claims ingested. Claims, 835 remittance data, and clinical data flow in through HL7, FHIR, X12 EDI, flat files, or direct integrations.
- Expected payment calculated. The pricing engine computes the expected reimbursement for every line item based on the applicable contract.
- Variance detected. The engine compares expected to actual paid amounts, including patient responsibility.
- Worklist routing. Variances flag automatically and route to the appropriate recovery worklist with full claim and contract context.
- Recovery and reporting. Staff or an outsourced recovery team pursue underpayments, appeal denials, and feed root cause data back into reporting.
This continuous loop is what turns a one-time audit into an ongoing revenue integrity program.
Software vs. outsourced services
There are two common operating models, and the right choice depends on staffing and complexity.
Software-only deployments give the in-house revenue cycle team a detection engine and worklist. The team owns the appeals and payer follow-up. This works well for organizations with experienced AR staff and bandwidth.
Outsourced zero balance review services pair the technology with a vendor's recovery specialists, who pursue payers, work appeals, and collect on the variances directly. This model is typically priced on a contingency basis, meaning the vendor takes a percentage of what they recover and the provider assumes no upfront risk. It works well for organizations that are short-staffed or facing complex multi-state payer footprints. Aspirion's overview of zero balance reviews provides a good primer on the outsourced model.
The most flexible vendors offer both, letting a provider run the platform in-house, outsource recovery, or mix the two as workload shifts.
Measurable ROI
The financial case is concrete. Published case studies show that:
- An orthopedics MSO identified $10.3 million in underpayments after deploying detection software.
- A radiology group validated $1.1 million in underpayments from a single payer.
- A community-care MSO recovered $160,000 from a single CPT code within three months of go-live.
Even at the low end of the underpayment range, a 20-physician group earning $13.3 million in net revenue is leaving $133,000 to $399,000 on the table every year. A 100-physician group is leaving $670,000 to $2 million. MD Clarity's zero balance account rate metric provides a useful KPI for tracking whether those gaps are closing over time.
How to evaluate zero balance review software
A short checklist for evaluation:

- Does the pricing engine simulate full payer adjudication logic, including modifier rules and lesser-of clauses?
- Does it operate at the charge level, not just the claim level?
- Does it ingest data from your existing PM, EHR, clearinghouse, and 835 feeds without heavy custom work?
- Does it provide drillable reporting by payer, contract, CPT, location, and provider?
- Does it include contract modeling for negotiations?
- Can the vendor also provide recovery services if your team is stretched?
- Are there published outcomes from organizations of similar size and specialty?
Frequently asked questions
What is the difference between a denial and an underpayment?
A denial is when the payer refuses to pay all or part of a claim and issues a remark code. An underpayment is when the payer processes the claim and pays - just less than the contracted amount, often with no notification.
How quickly does zero balance review software produce results?
Most providers see initial recoveries within three to six months of go-live, once contracts are digitized and claims data is flowing through the platform.
Is zero balance review the same as a payment variance report?
No. Payment variance reports inside a practice management system typically compare to a flat fee schedule and miss complex contract logic. Dedicated zero balance review software simulates the full adjudication process.
Does zero balance review software replace AR staff?
No. It removes manual spreadsheet work and surfaces the highest-value variances so staff can focus on appeals and recovery rather than detection.
How far back can zero balance review software look?
Most platforms can analyze claims data going back as far as it is retained, though filing and appeal deadlines vary by payer. Many recoveries are still viable on claims paid within the last 12 to 24 months.
What data does zero balance review software need?
At a minimum, the engine needs contracted allowed amounts at the CPT and modifier level, claim detail (CPT, modifiers, units, place of service, provider), 835 remittance data (allowed, paid, denial codes, patient responsibility), and current Medicare and Medicaid fee schedules.
Where to start with zero balance review software
For provider organizations that want a purpose-built platform, MD Clarity's RevFind is built specifically for zero balance review, underpayment detection, and contract optimization. RevFind digitizes payer contracts into a central repository and compares every remittance against contracted rates at the CPT, HCPCS, modifier, and site-of-service level. Its pricing engine simulates each payer's actual adjudication logic, including GPCI, lesser-of clauses, sequestration, modifier rules, bundling, mid-level differentials, and patient responsibility, so variances are accurate down to the charge.
When RevFind detects an underpayment, the account routes to a recovery worklist with the contract language and ERA detail attached. Reporting surfaces patterns by payer, contract, CPT, location, and provider, and the modeling engine lets revenue cycle leaders forecast the impact of proposed contract changes before negotiations. For organizations that prefer to outsource recovery, MD Clarity also pairs the platform with a team of payer reimbursement specialists who pursue appeals and collect on identified variances - making it one of the few end-to-end options that combines detection software and recovery services under one roof.
To see how RevFind performs against your own contracts and claims data, request a RevFind demo.
FAQs
Get paid in full by bringing clarity to your revenue cycle


.avif)
.svg)
.svg)


