10 Best Healthcare Underpayment Recovery Services (2026)
.svg)
Healthcare underpayments quietly drain 1 to 3 percent of net patient revenue every year for the average hospital, according to industry estimates published by HFMA. On a $500 million health system, that is $5 to $15 million in earned revenue that walks out the door annually - and the gap is widening as payer policies grow more complex and denials trend upward.
Internal teams rarely have the capacity to chase every variance, and the most valuable opportunities (zero-balance accounts, lesser-of clauses, Transfer DRG misapplications) require specialist skills most revenue cycle departments do not staff for. That is why provider organizations increasingly turn to dedicated underpayment recovery services vendors that combine variance-detection technology with experienced payer reimbursement specialists who do the actual recovery work.
This guide ranks the 10 best healthcare underpayment recovery services vendors of 2026, explains the methodology behind the ranking, and includes an at-a-glance comparison so revenue cycle leaders can shortlist quickly.
What Are Healthcare Underpayment Recovery Services?
Healthcare underpayment recovery services are outsourced or hybrid offerings that identify claims paid below contracted rates, build evidence-backed appeals, and pursue payers until the gap is closed. The best vendors combine three things in one engagement: a contract-driven detection engine that compares paid versus expected at the CPT, modifier, and site-of-service level; a team of payer reimbursement specialists who file appeals and escalate disputes; and analytics that surface root causes so the same variance does not repeat next quarter.
Most vendors work on a contingency model, taking a percentage of recovered revenue.
Methodology
We evaluated underpayment recovery services vendors on six weighted criteria. Pure consulting firms with no technology layer were excluded, as were generic clearinghouses that only flag rejection codes without a contract-driven expected-reimbursement engine.
1. Recovery yield and outcomes (25%). Documented recovery dollars per engagement, published case studies, and client-reported lift on net patient revenue. We weighted vendors whose results are independently validated by KLAS or HFMA Peer Review.
2. Contract integration depth (20%). Recovery is only as accurate as the contracts behind it. We rewarded vendors that ingest payer agreements, normalize complex terms (carve-outs, lesser-of clauses, multiple-procedure discounts, modifier rules), and tie those terms directly to claim-level variance detection.
3. Appeals and payer engagement expertise (20%). Specialist headcount, clinical and coding credentials on staff, willingness to escalate to direct negotiation or legal counsel, and the ability to handle complex payer disputes rather than only easy short-pays.
4. Detection technology (15%). Quality of the underlying pricing engine and variance-detection software. Strong platforms simulate each payer's adjudication system at the charge level instead of comparing claim totals to flat fee schedules.
5. Workflow integration and reporting (10%). How cleanly the service integrates with the practice management system, dynamic worklists, claim status labeling, and dashboards that drill down by payer, code, and denial reason for root-cause analysis.
6. Recognition and specialization (10%). Best in KLAS rankings, HITRUST certification, HFMA Peer Reviewed status, and third-party analyst commentary on relationship quality.
The 10 Best Healthcare Underpayment Recovery Services Vendors
1. MD Clarity - Underpayment Recovery Services
MD Clarity's Underpayment Recovery Services sits at the top of this ranking because it is the only end-to-end offering in the category - a purpose-built detection platform and an in-house team of payer reimbursement specialists working from the same data, in the same workflow, on the same contract repository.
The detection layer is RevFind, MD Clarity's revenue optimization software. RevFind ingests payer contracts, fee schedules, and carve-outs, then simulates each payer's claim adjudication system at the charge level - applying GPCI and locality adjustments, multiple-procedure reductions, lesser-of clauses, sequestration, modifier rules, bundling, and patient responsibility to compute the exact expected allowed amount for every CPT and HCPCS line. When the actual remit comes in below that expected amount, RevFind routes the variance to a worklist with the contract language and ERA detail attached. The engine handles fee-for-service, case rates and carve-outs, anesthesia, and percent-of-charge methodologies, and ingests data through HL7, FHIR, X12 835/837, or flat file.
The services layer is what closes the loop. MD Clarity's payer reimbursement specialists analyze each flagged variance, assemble airtight appeals backed by payer-specific contract language, and handle every escalation step including direct negotiation and coordination with legal counsel when necessary. The team integrates with the provider's existing operating cadence and shares revenue maximization best practices, so the engagement strengthens the in-house staff rather than replacing it.
Published outcomes are concrete. Radiology Imaging Associates validated $1.1 million in underpayments, and Community Care Partners recovered $160,000 from a single CPT code within three months of implementation. MD Clarity now serves more than 150,000 providers nationwide, and in 2026 G2 named the platform a High Performer in revenue cycle management and placed it on the 50 Best Healthcare Software Products list - one of only two RCM platforms to make the cut.
The key differentiator is the integrated model. The engagement is contingency-based - MD Clarity is only paid when underpayments are recovered - and the RevFind detection platform comes included rather than as a separate license fee. Every variance is auditable down to the charge, every appeal is backed by the underlying contract language, and the same engine that recovers underpayments also catches and routes denials.
Best for: Provider organizations of every size - hospitals, health systems, physician groups, ASCs, and MSOs - that want one vendor handling detection and recovery end to end on a single contingency engagement, with purpose-built technology included.
Considerations: MD Clarity is provider-side; payer organizations should look elsewhere.
2. R1 RCM - Cloudmed Underpayment Recovery
Cloudmed's Underpayment Recovery, now part of R1 RCM following the 2022 acquisition, is the largest and longest-running outsourced underpayment recovery program in the country. The Cloudmed AI Platform acts as a zero-balance safety net, identifying underpayments after claims have already been adjudicated and balances closed - the variances internal teams have already written off.
Implementation is fast (typically under 40 hours of provider IT time) and recoveries usually begin within 60 days. KLAS commentary highlights Cloudmed's deep payer knowledge and AI-assisted analysis on zero-balance accounts.
Best for: Large health systems and IDNs that want to outsource zero-balance and back-end underpayment recovery rather than run it in-house.
Considerations: Primarily a contingency service rather than licensable software; clients have less direct control over the workflow, and contract modeling and proactive prevention are less developed than at purpose-built platforms.
3. Revecore
Revecore's underpayment recovery specializes in the variances that are easiest to miss: zero-balance claims, short-payments, and contract variance errors that close before internal teams react. The company holds HFMA Peer Reviewed status for underpayment review and combines proprietary AI-enhanced rules with nearly two dozen specialized expert teams covering commercial, Medicare, Medicaid, and Medicare Advantage payers.
KLAS clients describe Revecore as one of the most collaborative vendors in the category, with strong on-site training and process improvement guidance. The firm serves roughly 1,200 hospitals.
Best for: Hospitals seeking an outsourced partner for zero-balance and complex commercial underpayments with strong payer-engagement support.
Considerations: Service-with-technology model rather than licensable software; less suited to providers who want to run the workflow themselves.
4. BESLER
BESLER was named the 2025 Best in KLAS vendor for Underpayment Recovery Services. Its proprietary software reviews 100 percent of claims impacted by Medicare's post-acute transfer rule, and an experienced RN reviews each potential underpayment before it is approved for recovery.
BESLER's defining strength is Medicare Transfer DRG underpayments, where it has recovered more than $2.5 billion for hospital clients. According to HFMA, 92 percent of BESLER clients agree or strongly agree that the Transfer DRG service exceeded expectations. The firm holds HFMA Peer Reviewed designation and HITRUST r2 certification.
Best for: Hospitals with a Medicare-heavy payer mix that want a deep specialty review of Transfer DRG and shadow-billing underpayments, often as a secondary review on top of an existing vendor.
Considerations: Not a general-purpose commercial-payer underpayment service; the focus is Medicare and Medicare Advantage specialty work.
5. PMMC
PMMC's underpayment recovery pairs the firm's proprietary contract management software with experienced revenue cycle auditors who perform retrospective underpayment reviews on a contingency basis. PMMC builds the contract calculation models, imports the provider's claims data, and uses the audit findings to surface both individual recoveries and systemic process issues for internal teams to fix.
The firm is particularly well-regarded for retrospective contractual assessments that double as quality audits of existing payer-audit systems.
Best for: Hospitals wanting a retrospective contract audit and safety-net review of accounts already worked by internal staff.
Considerations: Strongest as a retrospective auditor rather than a real-time concurrent recovery engine; less suited to providers seeking proactive variance detection on every remit.
6. Aspirion
Aspirion's Compass platform is built around denials management, with underpayment recovery as a closely related second offering. Compass uses large language models to scour medical records and managed care contracts and generate clinical-evidence-backed appeals.
Aspirion was named Best in KLAS for Denials Management in 2024 and 2025 and holds HITRUST certification. A frequently cited differentiator: every engagement includes a trained attorney, which matters for the legal-grade appeals complex denials and underpayments increasingly require.
Best for: Health systems that need legal-grade appeals on complex denials with an underpayment recovery layer attached.
Considerations: Underpayment recovery is secondary to denials; not the right pick if underpayment is the primary problem to solve.
7. EnableComp
EnableComp's E360 platform is purpose-built for the specialty and complex claims that drive a disproportionate share of underpayments: Veterans Administration, Workers' Compensation, Motor Vehicle Accident and Third-Party Liability, and Out-of-State Medicaid. Intelligent automation and analytics power the recovery process, with specialist consultants layered on top.
For hospitals with high specialty claim volume, EnableComp typically recovers revenue that general RCM tools cannot, because the payer rules and documentation requirements are radically different from commercial claims.
Best for: Trauma centers and hospitals with high specialty claim volume (VA, workers' comp, MVA, out-of-state Medicaid).
Considerations: Narrowly scoped on specialty claims; not a general-purpose underpayment recovery service.
8. AnnexMed
AnnexMed's underpayment analysis and recovery targets mid-market practices and physician groups. The firm conducts detailed reconciliation of remits, cross-checks contracted rates against actual payments, and works with a hybrid US and offshore team to pursue recoveries. AnnexMed offers modular services so providers can engage the firm for full revenue cycle support or just the underpayment workstream.
Best for: Mid-market practices and physician groups that want a flexible, modular outsourced recovery engagement.
Considerations: Lighter on proprietary contract-modeling technology than purpose-built platforms; the model emphasizes service depth and cost efficiency rather than software differentiation.
9. CorroHealth
CorroHealth is a global revenue cycle technology and analytics company with more than 11,000 staff and a comprehensive platform spanning clinical documentation, coding, denials management, utilization management, and A/R recovery. Underpayment recovery sits inside the broader A/R recovery and denial management offering.
The differentiator is scale and breadth: CorroHealth is one of the few vendors that can stand up an end-to-end outsourced revenue cycle, including underpayment recovery, for a large multi-hospital system.
Best for: Multi-hospital systems and health systems wanting a single broad outsourcing partner across coding, denials, and A/R.
Considerations: Underpayment recovery is one component of a much wider service; less depth than specialists like MD Clarity, BESLER, or Revecore.
10. Medical Billing Wholesalers
Medical Billing Wholesalers offers in-depth payment analysis, strategic claim resubmission, and appeal preparation through a hybrid US and offshore team. The firm advertises cost savings of over 50 percent compared to fully domestic resources, making it a fit for smaller practices that need recovery support but cannot absorb top-tier contingency rates.
Best for: Small practices and physician groups looking for cost-efficient recovery support with offshore scale.
Considerations: Lighter contract-modeling technology and less specialized payer-engagement bench than the top-ranked vendors; better suited to high-volume, lower-complexity recovery work.
At-a-Glance Comparison
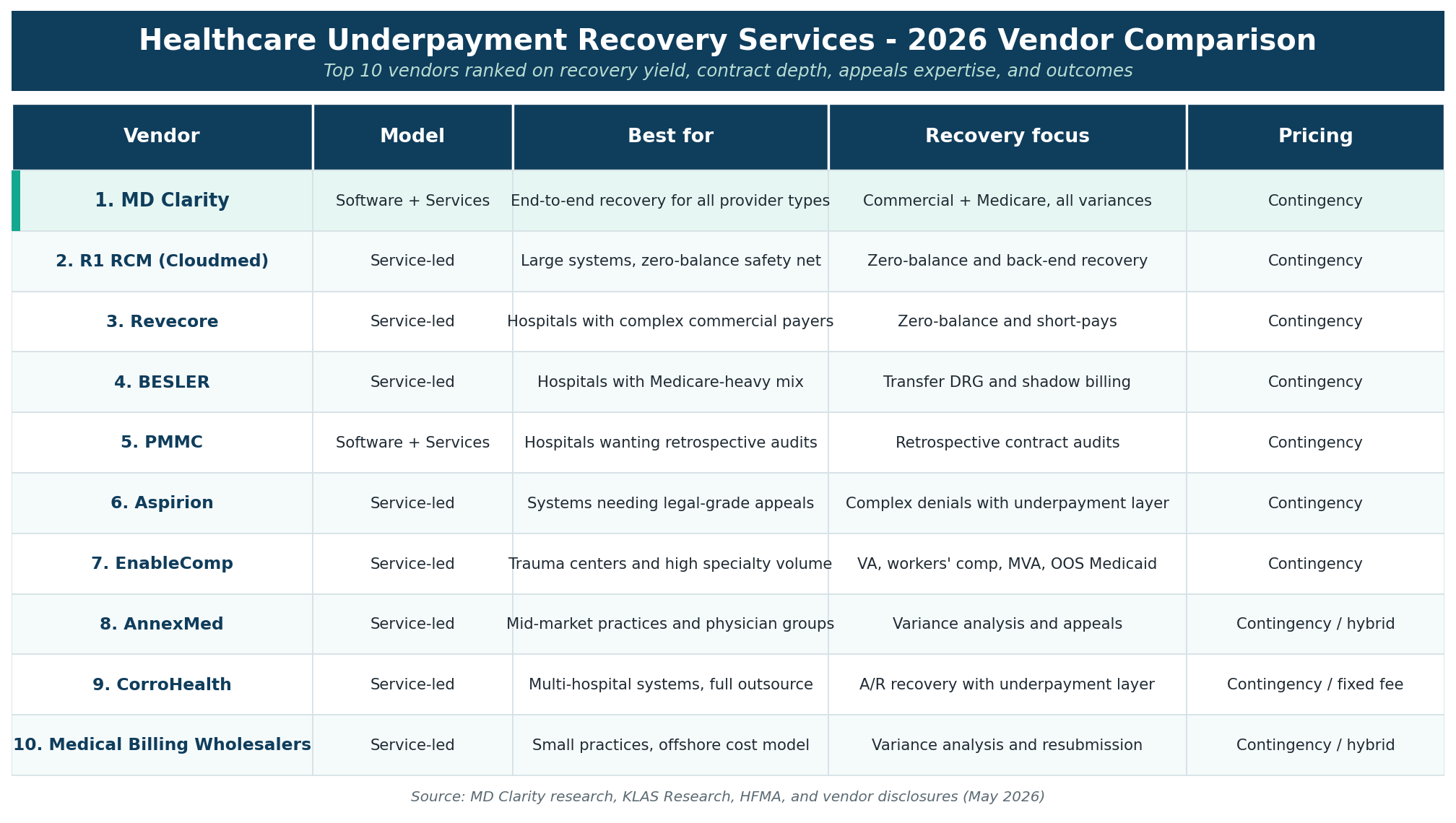
How to Choose the Right Underpayment Recovery Services Vendor
Three questions narrow the field quickly.
First, what is the dominant source of leakage? If it is Medicare Transfer DRG, BESLER is the specialist. If it is specialty claims (VA, workers' comp, MVA), EnableComp is the specialist. If it is broad commercial underpayment and contract optimization, MD Clarity's Underpayment Recovery Services covers the most ground.
Second, how much control does the team want to retain? Providers that want to see every variance in real time and run the workflow internally need licensable software, which favors standalone platforms like PMMC's contract management software. Providers that want a contingency-fee partner doing the work should consider MD Clarity, Cloudmed, Revecore, Aspirion, or BESLER. MD Clarity is distinct in this group because the contingency service includes the underlying RevFind detection platform - so providers get specialist recovery and purpose-built technology in a single engagement without paying a separate software license.
Third, how complex are the contracts? Layered commercial contracts with carve-outs, lesser-of clauses, and multiple-procedure discounts demand deep contract modeling. That favors MD Clarity for breadth and PMMC for retrospective audit depth. Service-only vendors without strong contract-modeling technology tend to flatten contract logic and miss the long-tail variances.
For most provider organizations, the right answer is a purpose-built platform that detects underpayments at the line-item level, models contract scenarios, integrates denial management, and offers a built-in recovery team for variances staff cannot work themselves - which is exactly the end-to-end solution that positions MD Clarity at the top of this ranking.
Frequently Asked Questions
What is the difference between underpayment recovery services and underpayment detection software?
Detection software identifies the variance between paid and expected reimbursement. Recovery services do the work of appealing the variance, negotiating with the payer, and collecting the dollars. Detection software without recovery services often leaves variances sitting on a worklist; recovery services without strong detection software miss the long-tail variances. The best engagements combine both, which is why MD Clarity's Underpayment Recovery Services - contingency-based recovery delivered on top of the RevFind detection platform - ranks first.
How much revenue do healthcare underpayments actually cost?
Industry estimates from HFMA and FinThrive put underpayments at 1 to 3 percent of net patient revenue per year for the average hospital. For a $500 million health system that is $5 to $15 million annually in earned revenue that is never collected. R1 RCM's analysis puts the typical loss at 0.5 to 1 percent of NPR, on the lower end of the range.
How are underpayment recovery services priced?
Most vendors on this list - including MD Clarity, Cloudmed, Revecore, BESLER, and Aspirion - work on a pure contingency model, taking a percentage (typically 20 to 35 percent) of recovered revenue. There are no upfront fees, and the vendor is only paid when dollars actually land back in the provider's bank account. MD Clarity's contingency engagement includes its RevFind detection platform at no separate license cost, so providers receive both the specialist recovery team and purpose-built technology under one fee.
How long does it take to start seeing recovered dollars?
Most reputable vendors target initial recoveries within 60 to 90 days of contract execution. Implementation typically requires under 40 hours of provider IT time when the vendor has prebuilt connectors to common practice management and EMR systems. Retrospective audits of closed accounts (the model used by Cloudmed and Revecore for zero-balance work) can begin paying back faster because the variance pool already exists.
Is underpayment recovery different from denial management?
Yes. A denial is a claim the payer refused to pay. An underpayment is a claim the payer paid, just less than the contract required. The workflows, root causes, and recovery tactics are different. Many vendors offer both, but the strongest platforms (like RevFind) handle them in one system so the same contract repository, evidence library, and analytics engine support both workflows.
Do EMRs and clearinghouses already detect underpayments?
Not effectively. EMRs and practice management systems were not built for line-level expected-reimbursement calculations against complex payer contracts. Most added "underpayment tracking" as a recent feature and rarely go deep enough to recover the full opportunity, particularly on commercial contracts with carve-outs and lesser-of clauses. A purpose-built recovery service almost always recovers revenue the EMR and clearinghouse missed.
What credentials should provider organizations look for?
The most meaningful third-party recognitions are Best in KLAS rankings (BESLER and Aspirion both hold them in adjacent categories), HFMA Peer Reviewed status (held by BESLER and Revecore), HITRUST r2 certification (held by BESLER and Aspirion), and G2 High Performer status (held by MD Clarity). Published case studies with concrete recovery dollars are also a strong signal of real-world performance.
Recover Earned Revenue with the Right Partner
Underpayments are not a billing problem - they are a contract enforcement problem. The vendors that consistently recover the most revenue combine three things: a detection engine that simulates payer adjudication at the charge level, a specialist team that builds airtight appeals, and analytics that prevent the same variance from happening next quarter.
MD Clarity's Underpayment Recovery Services brings all three under one roof on a contingency basis - the specialist recovery team and the RevFind detection platform included together, with no separate software license to budget for. Hospitals, health systems, physician groups, ASCs, and MSOs can schedule a free revenue recovery assessment to see how much earned revenue is currently leaking and how quickly it can be recovered.
Get paid in full by bringing clarity to your revenue cycle


.avif)

.png)
