symplr Contract vs MD Clarity PayerMonitor: Which Healthcare Contract Platform Is Right for You?
.svg)
symplr Contract and MD Clarity's PayerMonitor are two of the most recognized contract management platforms in healthcare - but they solve fundamentally different problems. Choosing between them isn't about which is "better." It's about which contract problem is costing your organization the most money.
This guide breaks down where each platform wins, how they compare on features, pricing, and implementation, and how to decide which one fits your needs. If your biggest exposure is compliance, vendor risk, and supply chain governance, symplr is likely the answer. If your biggest exposure is payer reimbursement and revenue leakage, PayerMonitor is built for exactly that.
TL;DR - The Quick Verdict
- Choose symplr Contract if you need an enterprise contract lifecycle management (CLM) system covering vendor, supply chain, and provider compensation agreements with deep Stark/AKS compliance tooling, HITRUST certification, and ERP integration.
- Choose MD Clarity PayerMonitor if your biggest contract challenge is payer agreements - managing reimbursement terms, catching underpayments, and turning contracts into revenue intelligence connected to denial management and recovery.
- Choose both if you're a large health system with mature contracting operations. They're complementary tools, not direct competitors. symplr governs the whole portfolio. PayerMonitor turns the most financially material contracts - payer agreements - into operational revenue intelligence.
At-a-Glance Comparison
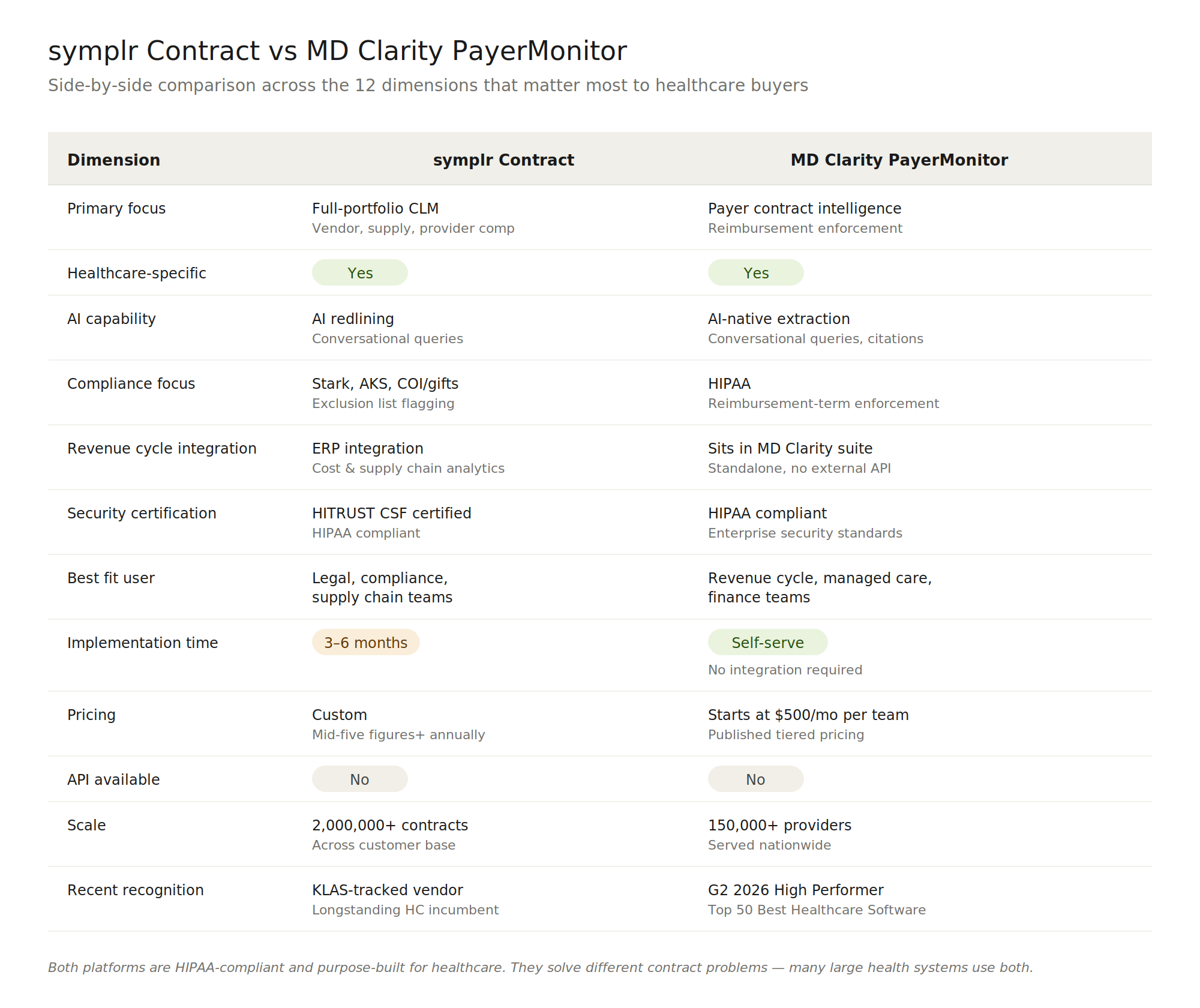
What symplr Contract Does Well
symplr Contract is the most established healthcare-specific CLM on the market and serves as the "system of record" for all contract types across a hospital or health system. Its position is enterprise-wide governance - covering supply chain agreements, vendor contracts, provider compensation, and BAAs from one repository.
Where symplr is strongest:
- Regulatory compliance breadth. Automated COI and gift tracking aligned to Stark Law and the Anti-Kickback Statute, exclusion list flagging for ineligible vendors and providers, and audit trails on every contract version. According to symplr, customers report up to a 60% reduction in compliance penalties through standardized language enforcement.
- HITRUST certification. symplr Contract is positioned as the only HITRUST-certified CLM purpose-built for healthcare - a meaningful credential for organizations with strict third-party assessment requirements.
- ERP integration. Tight links to financial systems give supply chain leaders the ability to track spend against contracted terms, monitor rebates, and prevent payments on expired agreements.
- AI-enabled redlining. AI scans contracts in minutes, flags high-risk clauses, and recommends revisions aligned to your legal playbooks - symplr cites up to 85% reduction in review time.
- Renewal alerting. Email and in-app alerts prevent costly auto-rollovers, with centralized visibility into renewal timelines across departments.
- Scale. symplr supports more than 2 million contracts across its healthcare customer base, with deep experience in large IDN deployments.
Where symplr's gaps show up:
- No reimbursement enforcement. symplr governs the contract document. It doesn't compare payer payments against contracted rates, model rate scenarios, or feed contract terms into denial recovery workflows. Those are revenue cycle problems that symplr was not designed to solve.
- Implementation length and cost. Public reviews and third-party comparisons cite a 3–6 month implementation timeline and pricing that "starts in the mid-five figures annually for large healthcare systems," requiring meaningful IT involvement.
- No API. Per public product listings, symplr Contract does not currently offer an API, which limits custom integrations beyond its native ERP and credentialing connectors.
- Best fit is legal/compliance/supply chain. Revenue cycle and managed care teams typically don't drive symplr deployments - and symplr's interface and workflows reflect that.
What MD Clarity PayerMonitor Does Well
PayerMonitor takes a fundamentally different approach. Rather than trying to govern every contract type across an enterprise, it goes deep on the most financially material contracts in healthcare: payer agreements. A single managed care contract can be worth hundreds of millions of dollars, yet most organizations still manage payer contracts in spreadsheets and shared drives. PayerMonitor exists to fix that.
Where PayerMonitor is strongest:
- Reimbursement-term extraction. The AI is trained on the language hospitals actually contend with - DRGs, carve-outs, lesser-of provisions, stop-loss, escalators, timely filing limits - and recognizes how different payers phrase the same term. Generic CLMs treat these as text strings; PayerMonitor treats them as structured operational data.
- Citation traceability. Every extracted term and AI-generated answer is linked to a snippet in the source contract. When a managed care director is preparing for a renegotiation, or a billing team is fighting a denial, they can verify the source instantly.
- Native integration with revenue recovery. PayerMonitor doesn't just store contracts - it connects them directly to MD Clarity's underpayment detection, denial management, contract modeling, and revenue recovery workflows. Contract terms flow into operational systems that catch revenue leakage in near real time.
- Self-serve onboarding. PayerMonitor requires no system integration to deliver value. Teams can sign up, upload contracts, and start using AI extraction immediately - time-to-value is essentially limited by how fast you can upload your contract files.
- Plain-language Q&A. Staff can ask natural-language questions about contract terms and get cited answers - without scrolling through 200-page PDFs.
- Third-party recognition. G2 named MD Clarity to its 2026 Best Software Awards on the Top 50 Best Healthcare Software Products list - one of only two revenue cycle platforms - alongside High Performer recognition in G2's Grid for revenue cycle management.
Where PayerMonitor's gaps show up:
- Not a full-portfolio CLM. PayerMonitor isn't built to manage vendor procurement contracts, supply chain agreements, BAAs, or provider compensation contracts. If you need one system to govern every contract in your organization, PayerMonitor is not that system.
- Doesn't replace Stark/AKS workflows. While HIPAA-compliant and built to enterprise standards, PayerMonitor isn't designed around the specific compliance workflows (COI tracking, gift logs, exclusion list monitoring) that symplr handles natively.
- Best fit is revenue cycle and managed care leadership. Legal-driven shopping processes that prioritize clause libraries and signature workflows will find PayerMonitor's positioning unfamiliar.
Side-by-Side: Feature Comparison
Contract centralization and search
Both platforms centralize contracts in a searchable repository with version control. symplr's strength is breadth - supporting every contract type across the enterprise. PayerMonitor's strength is depth - every payer contract is structured the same way, with reimbursement terms automatically extracted into comparable fields. If you've ever tried to compare timely filing limits across five payers in a generic CLM, you'll feel the difference immediately in PayerMonitor.
AI capabilities
Both platforms offer AI-powered conversational queries - meaning users can ask plain-language questions about their contracts and get answers from the AI without scrolling through document text. The platforms differ in what their AI is optimized to do beyond that. symplr's AI extends into redlining, flagging high-risk clauses against your legal playbook and accelerating contract review. PayerMonitor's AI is purpose-trained on reimbursement language and extracts structured terms (DRGs, carve-outs, lesser-of, stop-loss, escalators, timely filing limits) from each agreement, with every output linked to source citations for traceability. Both are useful; they're optimized for different jobs. symplr accelerates legal review. PayerMonitor accelerates revenue cycle decisions.
Compliance
symplr is the clear leader in regulatory contract compliance. Automated COI/gift tracking, exclusion-list flagging, and Stark/AKS-aligned workflows are deeply embedded. PayerMonitor focuses on HIPAA, secure architecture, and reimbursement enforcement. If the compliance question keeping you up at night is "are we exposing ourselves to Stark or AKS violations through provider relationships?" - that's symplr's territory. If it's "are we collecting what our payer contracts entitle us to?" - that's PayerMonitor's.
Revenue cycle integration
This is the biggest functional gap between the two. symplr integrates with ERP systems to support cost control and supply chain analytics - strong for finance and procurement use cases. PayerMonitor sits within MD Clarity's broader revenue optimization platform alongside RevFind (underpayment detection, denial management, contract modeling) and Clarity Flow (patient estimates) - so organizations using multiple MD Clarity products get a unified contract foundation that informs reimbursement enforcement and modeling decisions. Worth noting: PayerMonitor itself is intentionally standalone - there's no external API at this time and no EHR/ERP integration required to use it. Customers who want claim-level revenue cycle integration get that through MD Clarity's other products in the suite.
Security and certifications
Both platforms are HIPAA-compliant and built to enterprise security standards. symplr's HITRUST CSF certification is a notable differentiator for organizations whose third-party risk requirements explicitly require HITRUST. PayerMonitor's security architecture meets HIPAA and enterprise requirements, with vendor due diligence handled via standard SOC and security questionnaires.
Implementation and time-to-value
This is one of the most concrete differences between the two platforms. symplr Contract is an enterprise deployment - typically 3–6 months - that requires IT support, data migration planning, configuration of healthcare-specific workflows, and integration with ERP and credentialing systems. The result is a deeply embedded system of record across the organization, but the runway to first value is meaningful.
PayerMonitor takes the opposite approach: self-serve onboarding with no integration required. Teams subscribe, log in, and upload contracts. The AI begins extracting structured terms immediately, and time-to-value is essentially gated only by how fast the team can collect and upload its contract portfolio. There's no IT project, no integration timeline, and no professional services engagement required to start getting use out of the platform. For organizations frustrated by long enterprise software deployments, this is a substantively different model.
The trade-off is scope. symplr's longer timeline reflects its enterprise-wide governance posture; PayerMonitor's instant onboarding reflects its narrower, deeper focus on a single contract type.
Pricing
The two vendors take very different approaches to pricing transparency. symplr Contract uses fully custom pricing - public sources put it at mid-five figures and up annually for larger systems, with implementation, training, and ongoing support included.
MD Clarity publishes PayerMonitor pricing publicly across three tiers:
- Starter - $500/month per team (25 documents, 50 questions/month, unlimited users)
- Professional - $1,850/month per team (150 documents, 250 questions/month, unlimited users, priority support)
- Enterprise - custom pricing for larger health systems with high contract volume or complex requirements
Every tier includes the full AI feature set: term extraction, natural-language Q&A, citations, role-based access, and unlimited users. That structure makes PayerMonitor accessible to single-specialty groups and ASCs at the Starter level - a price point well below what enterprise CLMs typically reach - while still scaling up for IDNs at the Enterprise tier.
For an apples-to-apples comparison against your specific scope, request quotes from both vendors. PayerMonitor's published pricing makes initial budgeting and self-service procurement substantially easier, particularly for organizations that want to start with a defined pilot before scaling.
Use Case Decision Framework
Here's a practical way to figure out which platform - or combination - fits your organization.
Pick symplr Contract if you can answer "yes" to most of these:
- Your biggest contract risk is regulatory compliance (Stark, AKS, exclusion lists, gift/COI tracking)
- You manage thousands of vendor and supply chain agreements alongside provider contracts
- HITRUST certification is a third-party risk requirement
- Supply chain, legal, or compliance leadership owns the buying decision
- You have IT bandwidth and budget for a 3–6 month enterprise implementation
- ERP integration is a hard requirement
Pick MD Clarity PayerMonitor if you can answer "yes" to most of these:
- Your biggest contract risk is payer reimbursement and revenue leakage
- You're managing payer agreements in spreadsheets, shared drives, or a generic system that wasn't built for them
- You want contract terms to drive operational outcomes (catching underpayments, supporting appeals, modeling rate negotiations)
- Revenue cycle, managed care, or finance leadership owns the buying decision
- You need to be live immediately - self-serve onboarding, no IT project
- You want a platform that grows into broader revenue optimization (denial management, recovery services)
Use both if:
- You're a large health system or IDN where contract risk spans both compliance/vendor and payer reimbursement
- You have differentiated buying centers (legal/compliance owns CLM; managed care/finance owns payer contract intelligence)
- Your annual contract value at risk on either dimension justifies dedicated tooling
This isn't an unusual conclusion. The largest health systems frequently maintain both an enterprise CLM and a specialized payer contract intelligence platform because the workflows, owners, and outcomes are genuinely distinct.
Customer Profile: Who Buys What
symplr Contract customers are typically large hospitals and health systems with mature procurement and compliance functions. The platform's pricing and implementation requirements push it toward organizations with hundreds or thousands of vendor relationships, dedicated supply chain leadership, and a need for enterprise-wide contract governance. Reviews on Capterra and Software Advice frequently cite the platform as "designed specifically for the healthcare industry" but flag pricing as the most common drawback.
MD Clarity customers range from large hospitals to mid-sized physician groups and management services organizations (MSOs). The common thread is a sophisticated revenue cycle or managed care function that views payer contracts as financial instruments - not just legal documents. MD Clarity now serves more than 150,000 providers nationwide, and its broader revenue optimization platform appeals to organizations that want contract intelligence connected directly to claim-level revenue recovery.
Frequently Asked Questions
Are symplr Contract and MD Clarity PayerMonitor direct competitors?
Not really. They overlap on contract centralization, but their core jobs are different. symplr Contract is a full-portfolio CLM emphasizing compliance and vendor governance. PayerMonitor is a specialized payer contract intelligence platform that ties to reimbursement enforcement. Many large health systems use both.
Can MD Clarity PayerMonitor replace a CLM?
Not for vendor, supply chain, or provider compensation contracts. PayerMonitor is purpose-built for payer agreements and the reimbursement workflows attached to them. If your biggest contract problem is payer reimbursement, PayerMonitor solves it deeply. If you need to govern every contract type from one system, you need a CLM.
Can symplr Contract handle payer contracts?
Yes - payer agreements can be stored and tracked in symplr Contract like any other document. What symplr doesn't do is extract structured reimbursement terms (DRGs, lesser-of, carve-outs, stop-loss, escalators, timely filing limits), benchmark them across payers, model rate scenarios, or feed them into underpayment detection. Those are revenue cycle capabilities that require purpose-built tooling.
Which platform deploys faster?
PayerMonitor, by a wide margin. It's a self-serve platform with no integration requirement - teams sign up, upload their contract files, and the AI begins extracting structured terms right away. There's no IT project or professional services engagement needed to get going. symplr Contract's enterprise scope typically requires 3–6 months for full deployment, including data migration, workflow configuration, and ERP integration.
Which platform has better AI?
They're optimized for different things. Both platforms offer conversational AI for natural-language contract queries. Beyond that, symplr's AI is strong at redlining contracts against legal playbooks. PayerMonitor's AI is purpose-trained on reimbursement language, with citation-traceable outputs and structured term extraction. The "better" AI depends on which job you're trying to do.
How much do they cost?
symplr Contract uses custom pricing, typically starting in the mid-five figures annually for large health systems. PayerMonitor publishes its pricing: Starter at $500/month per team, Professional at $1,850/month per team, and custom Enterprise pricing - all tiers include unlimited users and the full AI feature set, with tiers differing on document count and question volume. Request quotes from both for an apples-to-apples comparison against your specific scope.
Is one HIPAA-compliant and the other not?
Both are HIPAA-compliant. symplr Contract additionally holds HITRUST CSF certification, which can matter for organizations whose third-party risk frameworks explicitly require HITRUST.
Which platform integrates with my EHR or ERP?
symplr Contract emphasizes ERP integration for cost control and supply chain analytics. PayerMonitor is intentionally standalone - it doesn't require or offer EHR/ERP integration, which is what makes its self-serve onboarding possible. If you're already using MD Clarity's broader revenue platform (RevFind, Clarity Flow), PayerMonitor sits naturally alongside those products. For deeper claim-level integration with your EHR or billing system, that's handled by other modules in the MD Clarity platform rather than PayerMonitor itself.
The Bottom Line
If you're trying to pick between symplr Contract and MD Clarity PayerMonitor, start with the question: "What's the contract problem actually costing us money?"
If the answer is regulatory exposure, vendor risk, or supply chain governance, symplr is the right tool. If the answer is payer reimbursement, underpayments, or revenue leakage on managed care agreements, PayerMonitor is built for that exact problem and connects directly into the revenue cycle workflows that close the loop.
For most provider organizations, the bigger financial lever is payer contracts. A single underpaid contract clause can leak millions of dollars per year - and unlike compliance fines, that leakage is invisible without the right tooling. That's the gap PayerMonitor was built to close.
Ready to see PayerMonitor in action? Request a demo from MD Clarity to see how AI-native payer contract management can turn your agreements into recovered revenue.
Get paid in full by bringing clarity to your revenue cycle


.avif)


