The 10 Best Payer Contract Management Software Vendors in 2026
.svg)
Payer contracts are the largest financial lever in any provider organization. A single managed care agreement can be worth hundreds of millions of dollars in annual revenue, run thousands of pages across amendments and fee schedules, and tie directly to whether a hospital gets paid correctly on every claim it submits. Yet most provider organizations still manage their payer agreements in spreadsheets, shared drives, or generic contract lifecycle management (CLM) software that was built for sales contracts, NDAs, and procurement deals - not reimbursement terms or payer behavior.
Payer contract management software is the category designed to fix that gap. The best platforms extract structured reimbursement terms (DRGs, carve-outs, lesser-of provisions, stop-loss, escalators, timely filing limits), benchmark them across payers, support renegotiations, and connect contract data to revenue cycle workflows that catch underpayments before they become permanent revenue losses.
This guide ranks the ten best payer contract management software vendors in 2026 - including the few platforms genuinely purpose-built for payer agreements, the healthcare CLMs that can handle payer contracts as part of broader contract operations, and the general-purpose CLMs healthcare organizations sometimes evaluate. We weigh payer-specific capabilities, AI depth on reimbursement language, integration with revenue cycle workflows, and - critically - whether the platform actually moves the needle on revenue or just stores agreements in a fancier filing cabinet.
TL;DR - The Best Payer Contract Management Software at a Glance
- MD Clarity PayerMonitor - Best overall for payer contract management. Purpose-built, AI-native, ties contracts directly to underpayment detection and revenue recovery.
- Icertis - Best for Fortune-class enterprises with budget for an enterprise CLM that includes payer contract analytics as part of a broader healthcare vertical solution.
- symplr Contract - Best for large hospitals managing payer contracts alongside supply chain and provider compliance.
- Ntracts - Best for compliance-led health systems where payer contracts sit alongside provider credentialing and policy workflows.
- Conga CLM - Best for Salesforce-driven enterprises wanting payer contracts inside their broader Revenue Lifecycle Management platform.
- CobbleStone Contract Insight - Best for highly configurable enterprise CLM with the option for on-premises deployment.
- Ironclad - Best for legal-driven organizations using Ironclad enterprise-wide that need a basic payer contract repository.
- DocuSign CLM - Best for organizations already standardized on DocuSign that want to extend into post-signature payer contract tracking.
- Concord - Best for SMB and mid-market healthcare organizations needing AI-assisted general CLM with payer contracts as one of many contract types.
- ContractSafe - Best for fast-deploying contract repository when your primary need is searchable storage rather than reimbursement enforcement.
Methodology: How We Ranked These Platforms
We evaluated 25 contract management vendors against six weighted criteria specifically relevant to payer contract management for provider organizations. Vendors had to be capable of storing and managing payer agreements - though most general CLMs only do this superficially. Pure-play e-signature tools and document repositories without contract intelligence were excluded.
Payer contract specificity (35%). Was the platform built for payer agreements, or does it treat them like any other document? We examined whether the AI is trained on reimbursement language, whether the platform recognizes how different payers phrase the same term (DRGs, lesser-of, stop-loss, escalators, timely filing limits), and whether structured payer contract data is the platform's primary output. Platforms purpose-built for payer contracts scored highest; general CLMs that can store payer agreements scored lowest.
Reimbursement enforcement and revenue impact (30%). Contract management that ends at "filed correctly" leaves money on the table. We weighted features that detect underpayments, model contract scenarios, benchmark payer rates, and surface revenue exposure tied to specific contract language. We also looked at whether the platform connects to revenue cycle workflows - claim-level integration, denial management, recovery services - that close the loop between contract terms and recovered dollars.
AI for payer contract language (15%). We looked beyond marketing copy to evaluate whether the AI is grounded in healthcare reimbursement data, whether it cites source language for traceability when answering questions, and whether it can normalize how different payers express the same concept. Generic LLM wrappers and AI built for sales contracts were marked down.
Compliance and security (10%). HIPAA, SOC 2 Type 2, audit trails, role-based access controls. Table stakes for any platform handling payer contracts.
Implementation and time-to-value (5%). A six-month implementation that requires three FTEs is a different product than a 30-day rollout. We adjusted scores for total cost of ownership and realistic time to first useful output.
Customer evidence (5%). KLAS reports, public case studies, named provider customers, and platform breadth (number of providers served) factored in here.
We did not accept vendor sponsorship for placement. Pricing reflects publicly available information and vendor-disclosed ranges as of April 2026.
1. MD Clarity PayerMonitor - Best Overall for Payer Contract Management
MD Clarity's PayerMonitor earns the top spot because it is the only platform on this list designed from the ground up for payer contract management - the contracts that actually determine whether a healthcare provider organization gets paid correctly. Every other vendor here is either a generic CLM that can store payer agreements, a healthcare CLM focused on compliance rather than reimbursement, or an enterprise platform with payer features layered on as a vertical solution.
That distinction matters enormously. PayerMonitor's AI is trained on the language hospitals actually contend with - DRGs, carve-outs, lesser-of provisions, stop-loss, escalators, timely filing limits, renewal and termination clauses, related agreements - and recognizes how different payers phrase the same term. Where a generic CLM treats reimbursement terms as searchable text, PayerMonitor treats them as structured operational data that flows into downstream revenue workflows.
The platform's outputs are fully traceable. Every extracted term and AI-generated answer links back to a citation snippet in the source contract, which matters enormously when a managed care director is preparing for a renegotiation or a billing team needs to fight a denial. PayerMonitor also supports plain-language Q&A - staff can ask questions like "what's our timely filing limit with Cigna?" and get cited answers in seconds, rather than scrolling through 200-page PDFs.
Where PayerMonitor really separates itself from the rest of this list is its integration into MD Clarity's broader revenue optimization platform. Payer contracts feed directly into payer benchmarking, scenario modeling, underpayment detection, denial management, and recovery workflows. You're not just storing payer contracts - you're using them as operational tools that recover revenue.
That depth of focus shows up in third-party recognition. MD Clarity now serves more than 150,000 providers nationwide, and in 2026, G2 named the platform a High Performer in revenue cycle management and placed it on its 50 Best Healthcare Software Products list - one of only two revenue cycle management platforms to make the cut. Its decade-long track record capturing managed care complexity is reflected in how the AI behaves.
Best for: Provider organizations - hospital systems, physician groups, ASCs, specialty practices - whose biggest contract risk is payer reimbursement and revenue leakage.
Pros:
- Purpose-built for payer contract management, not adapted from generic CLM
- AI grounded in real RCM workflows with citation-backed outputs
- Native integration with underpayment detection, modeling, and recovery
- Self-serve onboarding with no IT project required
- HIPAA compliant with secure architecture
- Recognized by G2 in 2026 as a High Performer and one of the 50 Best Healthcare Software Products
- Solves the actual revenue problem, not just the storage problem
- Transparent published pricing starting at $500/month per team
Cons:
- Not designed for vendor procurement, supply chain, or general business contracts
- Better fit for revenue cycle, managed care, and finance teams than for legal/compliance-only buyers
- No external API at this time (standalone product)
Pricing: Published tiered pricing: Starter at $500/month per team, Professional at $1,850/month, custom Enterprise. Every tier includes unlimited users and the full AI feature set.
2. Icertis - Best Enterprise CLM with Payer Contract Analytics
Icertis is one of the most powerful enterprise CLMs in any industry, and the only platform on this list besides MD Clarity that explicitly markets payer contract analytics. In 2022, the company launched Icertis Contract Intelligence (ICI) for Healthcare Providers, a vertical solution with pre-configured contract types and AI models for payer, physician, supplier, and clinical education agreements - including dashboards for benchmarking payer contracts and AI-powered analysis of reimbursement terms.
The trade-off is implementation. Icertis deployments typically take 6-12 months with technical staff or consultants required to configure the platform. First-year costs typically run $200,000-$300,000 when licensing, implementation, and training are combined - meaningfully above the CLM market average. For Fortune-class health systems with the budget and IT capacity, Icertis is exceptionally capable. For most provider organizations, it's overkill for the payer contract management use case alone.
Best for: Fortune-class health systems and IDNs with enterprise-wide contracting complexity beyond just payer agreements.
Pros: Real payer contract analytics in healthcare provider vertical solution; deep configurability; strong enterprise integrations (SAP, Microsoft, Salesforce, Workday); Gartner Magic Quadrant Leader. Cons: 6-12 month implementation; first-year costs typically $200K+; payer contract handling is a vertical layered on horizontal CLM, not the platform's core focus.
3. symplr Contract - Best Healthcare CLM for Hospitals Managing Payer Plus Other Contracts
symplr Contract is the most established healthcare-specific CLM on the market, with more than two decades of experience in hospital contracting. While its primary strengths are supply chain agreements, provider contracts, and Stark/AKS compliance workflows, payer contracts can be stored and tracked alongside other healthcare contract types. It's not a payer contract management platform specifically, but for organizations that want healthcare-aware contract operations covering payer agreements as part of a broader portfolio, symplr is a credible choice.
Standout capabilities include AI-enabled redlining, automated COI and gift tracking aligned with Stark and AKS, exclusion-list flagging for ineligible vendors and providers, and ERP integration for financial control. What symplr doesn't do is extract structured payer reimbursement terms, benchmark across payers, model rate scenarios, or feed contract terms into underpayment detection.
Best for: Large hospitals and IDNs managing payer contracts alongside supply chain, provider compensation, and compliance workflows.
Pros: Deepest healthcare regulatory tooling; mature AI redlining; strong renewal alerting; HITRUST CSF certified. Cons: Not a dedicated payer contract management platform; no reimbursement-term enforcement; enterprise pricing; setup requires significant IT involvement.
4. Ntracts - Best for Compliance-First Health Systems That Also Manage Payer Contracts
Ntracts is built specifically around healthcare contracting, compliance, and policy workflows - founded by Hall Render, one of the country's leading healthcare law firms. It serves hospitals, physician groups, FQHCs, and payer organizations, with particular strength in provider onboarding, credentialing, and compensation management. Payer contracts can be stored and tracked in Ntracts, but the platform's strength is compliance and provider services rather than payer reimbursement enforcement.
The platform recently exceeded the national software average by five-plus points in KLAS Research, reflecting strong responsiveness and customer support. Automation is tuned to Stark Law, AKS, and other healthcare-specific standards.
Best for: Health systems and physician groups where compliance and provider contracts are the primary focus and payer contracts are managed as part of a broader portfolio.
Pros: Healthcare-native by design; strong KLAS scores; real expert support; CIA-tested compliance workflows. Cons: Not a dedicated payer contract management platform; no reimbursement-term extraction; no native revenue cycle integration.
5. Conga CLM - Best for Salesforce-Driven Enterprises with Payer Contracts in a Broader Portfolio
Conga CLM is a strong choice for mid-to-large enterprises (especially those standardized on Salesforce) that need unified Revenue Lifecycle Management - pricing, quoting, contracting, document automation, and eSignature - on one platform. Payer contracts can be stored and tracked alongside sales contracts, vendor agreements, and other contract types, with Conga's AI handling general extraction and risk scoring. Conga has 10,000+ customers and 6.4M+ users globally, making it one of the largest CLM platforms by footprint.
What Conga doesn't do is extract structured payer reimbursement terms specifically, benchmark them across payers, or connect contracts to claim-level revenue cycle workflows. Conga's "Revenue Lifecycle Management" refers to the commercial sales process, not healthcare revenue cycle management.
Best for: Mid-to-large enterprises with Salesforce as their system of record that want unified contract operations across all contract types including payer.
Pros: Deep Salesforce integration; broad Revenue Lifecycle Management suite; G2 Leader for CLM; mature platform with 19+ years in market. Cons: Not healthcare-specific; no payer reimbursement enforcement; some reviewers describe AI as "limited"; learning curve for new users; 6 weeks to several months implementation.
6. CobbleStone Contract Insight - Best Configurable Enterprise CLM with On-Premises Option
CobbleStone consistently appears on healthcare CLM shortlists and offers strong configurability for organizations that want to tailor every workflow. With 30+ years in market, the platform covers contract authoring, e-signatures, obligation tracking, vendor management, eSourcing, and procurement - all powered by its proprietary VISDOM AI engine. Payer contracts can be stored and managed within this broader procure-to-pay framework.
CobbleStone offers both SaaS and on-premises deployment options - rare in modern CLM and meaningful for organizations with strict data residency requirements. The platform also offers a 30-day free trial, which is unusually generous for enterprise CLMs.
Best for: Enterprises that want highly configurable contracting across procure-to-pay and have IT capacity to support configuration.
Pros: Deep configurability; on-premises and SaaS deployment options; 30-day free trial; native iOS/Android mobile apps; strong customer support reputation; 5/5 G2 rating. Cons: Not a dedicated payer contract management platform; no reimbursement-term enforcement; learning curve flagged by reviewers; healthcare workflows require build-out.
7. Ironclad - Best General CLM for Legal-Driven Healthcare Organizations
Ironclad is the CLM legal teams reach for when they want flexible workflow design and modern AI without enterprise complexity. The recent launch of Jurist - an agentic AI for legal contract review - positions Ironclad at the forefront of AI-native CLM. Payer contracts can be stored and managed alongside NDAs, sales agreements, and vendor contracts using Ironclad's flexible workflow engine.
Ironclad isn't healthcare-specific, and there's no native payer reimbursement extraction or revenue cycle integration. For provider organizations whose legal team already runs Ironclad enterprise-wide and wants to consolidate payer contracts into the same platform, it's a credible option - though most healthcare buyers focused specifically on payer contract management will find purpose-built tools more fit-for-purpose.
Best for: Provider organizations where legal owns contract operations enterprise-wide and wants payer contracts in the same workflow as other contract types.
Pros: Excellent UX; flexible no-code workflows; Jurist agentic AI; strong third-party integrations; HIPAA, SOC 2, ISO 27001, GDPR certified. Cons: Not healthcare-specific; no native payer reimbursement-term extraction; no revenue cycle integration; total annual contract values typically $30K-$250K+.
8. DocuSign CLM - Best for DocuSign-Standardized Organizations Adding Payer Contract Tracking
If your organization already runs e-signatures through DocuSign, DocuSign CLM is the natural extension when contract needs grow beyond signing. It supports drafting, approvals, and ongoing contract tracking with template-based creation. DocuSign offers a HIPAA-compliant tier, and recent investments in DocuSign IAM and AI Agents have added meaningful AI capabilities to the platform.
DocuSign CLM is not built for payer contract management specifically. There's no structured reimbursement-term extraction, no payer benchmarking, and no revenue cycle integration. Total cost of ownership often runs higher than expected once implementation, integration, training, and per-user pricing are factored in.
Best for: Healthcare organizations already standardized on DocuSign that want to extend into post-signature payer contract tracking as part of a broader CLM rollout.
Pros: Industry-leading native eSignature; familiar interface for existing DocuSign customers; HIPAA-compliant tier; strong Salesforce integration. Cons: Not built for payer contract management; per-user pricing scales unfavorably for healthcare departments needing broad access; total 3-year spend often doubles base license; no free trial for CLM.
9. Concord - Best AI-Native General CLM for SMB and Mid-Market Healthcare
Concord is a cloud-based CLM with AI Copilot and the recently-launched Horizon AI-first conversational platform - one of the more modern UIs in the CLM space. The platform includes unlimited eSignature on every plan and offers transparent published pricing starting at $399/month for 5 users. Concord serves 1,500+ SMB and mid-market organizations, with healthcare representing a small portion of their customer base.
Payer contracts can be stored and managed alongside sales agreements and other contract types using Concord's AI extraction and conversational queries. There's no payer-specific term extraction, no reimbursement enforcement, and no revenue cycle integration - Concord is a general-purpose CLM, not a healthcare-specific platform.
Best for: SMB and mid-market healthcare organizations needing AI-assisted CLM across many contract types, with payer contracts as one part of broader contract operations.
Pros: Modern AI-native UI; unlimited eSignature on every plan; transparent published pricing; fast deployment (1 day to weeks); strong SMB user satisfaction. Cons: Not healthcare-specific (only ~7% healthcare customers); no payer reimbursement enforcement; per-seat pricing scales unfavorably for healthcare departments; reviewers note AI depth limits versus specialized platforms.
10. ContractSafe - Best Fast-Deploy Repository for Smaller Practices
ContractSafe is SOC 2 and HIPAA compliant, with custom roles, OCR-powered search, an AI assistant ([AI]ssistant) for general data extraction, and unlimited users on every plan. Crucially, it offers a 7-day free trial and most teams can be live in under 30 minutes - meaningful for smaller practices and specialty groups that need to centralize contracts without an enterprise CLM project.
ContractSafe markets to healthcare and serves many healthcare organizations, but the platform itself is industry-agnostic. Payer contracts can be stored and searched, but ContractSafe doesn't extract structured reimbursement terms, benchmark across payers, or integrate with revenue cycle workflows. Per their own comparison framing, ContractSafe is not built for payer-contract analytics.
Best for: Small to mid-sized practices, specialty groups, and ASCs whose immediate problem is "we have contracts everywhere" rather than payer reimbursement enforcement.
Pros: Fast deployment (under 30 minutes claimed); intuitive search; transparent pricing; unlimited users on every plan; 7-day free trial; SOC 2 + HIPAA compliant. Cons: Not built for payer contract management; general-purpose AI without healthcare reimbursement training; limited workflow customization; AI quality flagged for improvement by some reviewers.
At-a-Glance Comparison
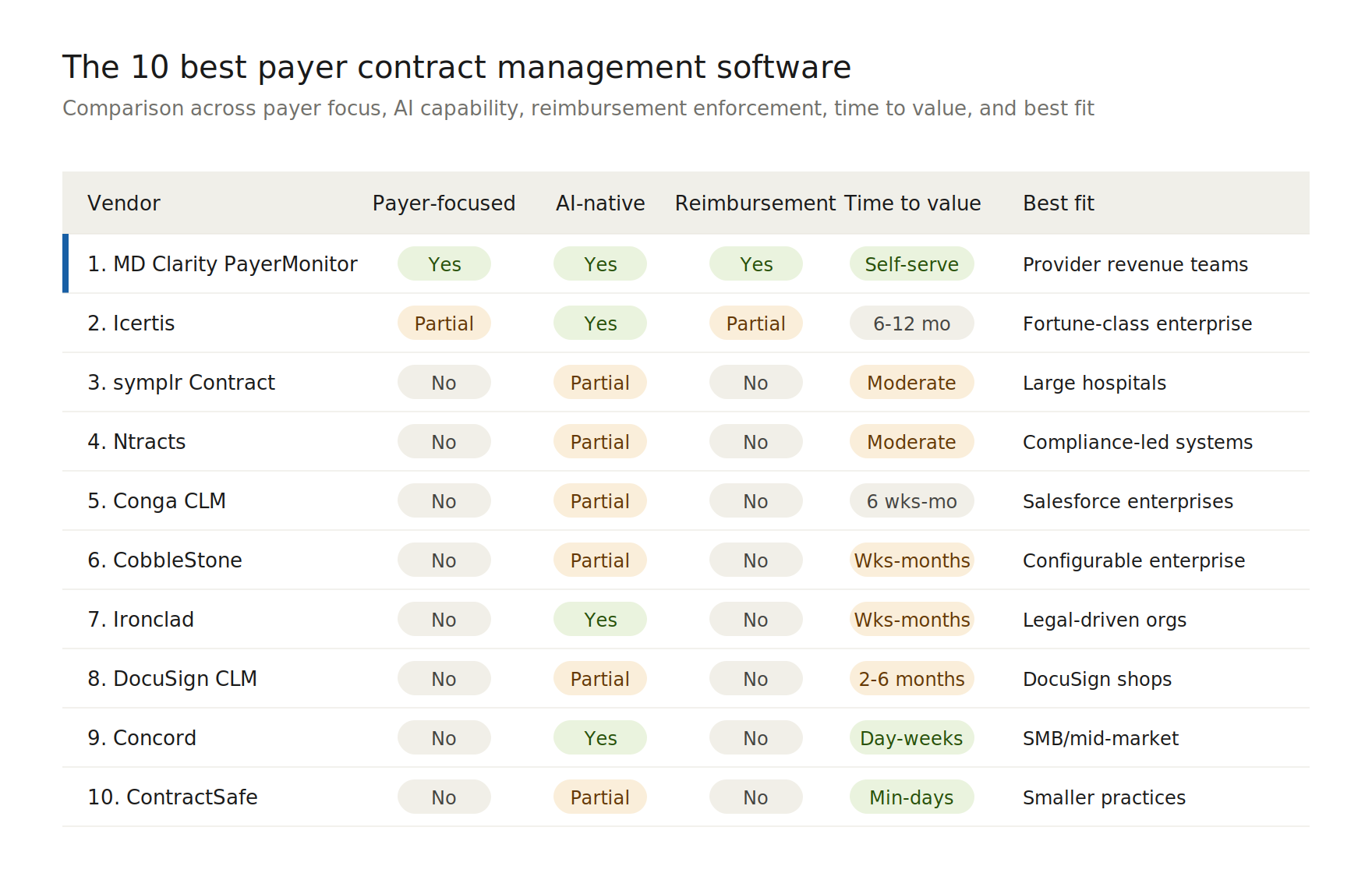
How to Choose the Right Payer Contract Management Software
Three questions will narrow your shortlist faster than any feature comparison.
Is payer reimbursement actually your biggest contract problem? If yes, a purpose-built payer contract management platform (MD Clarity PayerMonitor) will deliver more value than any horizontal CLM, regardless of how mature or well-reviewed the horizontal platform is. If your contract problem is broader - mixing payer agreements with vendor contracts, NDAs, and procurement - a healthcare CLM (symplr, Ntracts) or enterprise CLM (Icertis, Conga) becomes more relevant.
Who owns payer contracts in your organization? Revenue cycle, managed care, and finance teams gravitate toward MD Clarity. Legal and procurement teams gravitate toward enterprise CLMs (Icertis, Ironclad, Conga). Compliance teams gravitate toward healthcare CLMs (symplr, Ntracts). The owner of the implementation usually predicts which platform sticks - and revenue cycle teams especially benefit from purpose-built tools that match their workflows.
How fast do you need to be live? If the answer is 30-60 days, eliminate Icertis and most enterprise CLMs. PayerMonitor (self-serve), ContractSafe (under 30 minutes claimed), and Concord (1 day to weeks) are designed for fast deployment. If you have IT bandwidth for a 6-month rollout, the configurability advantages of enterprise platforms start to pay off - though only for organizations that need them.
Frequently Asked Questions
What is payer contract management software?
Payer contract management software is a specialized category of contract management platforms designed specifically for managing agreements between healthcare providers and payers (insurance companies, government payers, managed care organizations). The best platforms extract structured reimbursement terms (DRGs, lesser-of provisions, stop-loss, escalators, timely filing limits), benchmark them across payers, support renegotiations, and connect contract data to revenue cycle workflows that catch underpayments.
How is payer contract management software different from general CLM?
General CLM software treats every contract the same - it stores documents, tracks renewal dates, and may offer basic AI for clause extraction. Payer contract management software is purpose-built for the unique challenges of payer agreements: hundreds of payer-specific terms expressed differently across contracts, reimbursement-driven financial impact (often millions of dollars), and the need to feed contract data into claim-level revenue cycle systems for underpayment detection. A general CLM can store payer contracts; a payer contract management platform actively manages reimbursement.
Why do healthcare providers need payer contract management software specifically?
Payer contracts are typically the largest financial lever in any provider organization. A single underpaid contract clause can leak millions of dollars per year in revenue - invisible without the right tooling. Generic CLMs and even healthcare-specific CLMs that focus on Stark/AKS compliance don't address this gap. Payer contract management software is purpose-built to surface reimbursement terms, model rate scenarios, and connect contracts to underpayment recovery.
What's the difference between payer contract management software and revenue cycle software?
Payer contract management software stores and structures payer agreements and extracts reimbursement terms. Revenue cycle management (RCM) software manages claims, payments, and denials. The most powerful approach for provider organizations connects the two - so contract terms flow directly into underpayment detection, denial management, and recovery workflows. That's the gap MD Clarity's platform was designed to close, with PayerMonitor handling contract management alongside RevFind for underpayment detection.
Can I use a general CLM for payer contract management?
You can store payer contracts in any CLM, but you'll lose the structured reimbursement-term extraction, payer benchmarking, and revenue cycle integration that purpose-built platforms provide. For organizations whose primary contract problem is payer reimbursement, a general CLM is essentially expensive document storage. For organizations managing payer contracts as one of many contract types, a healthcare CLM like symplr or Ntracts can be a reasonable choice.
How long does payer contract management software implementation take?
It varies dramatically by platform. Self-serve payer contract management platforms like PayerMonitor can be live in days - teams subscribe, upload contracts, and AI extraction begins immediately. Healthcare-specific CLMs like Ntracts or symplr typically take 60-120 days. Enterprise CLMs like Icertis routinely take 6-12 months. The implementation timeline often correlates with platform breadth: focused products deploy faster, configurable platforms deploy slower.
What does payer contract management software cost?
Pricing models vary widely. Purpose-built payer contract management platforms like PayerMonitor publish transparent pricing starting at $500/month per team with unlimited users. Healthcare-specific enterprise CLMs typically use custom pricing tied to contract volume and modules - often starting in the tens of thousands annually for mid-sized organizations. Enterprise CLMs like Icertis or Ironclad typically start at $30K-$200K+ first-year, scaling with users and integrations.
Can AI really extract reimbursement terms accurately?
It depends on whether the AI was trained on healthcare reimbursement contracts specifically. Generic LLM wrappers struggle with payer-specific phrasing variations and reimbursement terminology - "lesser-of," "stop-loss," "carve-outs," and "DRGs" mean different things in different payer contracts. Platforms purpose-built for payer contracts (like PayerMonitor) combine frontier LLMs with domain-specific document analysis models trained on real reimbursement language, making them substantially more accurate at extracting structured terms and citing source language than general-purpose CLM AI.
The Bottom Line
The best payer contract management software for a provider organization depends on what's actually driving the buying decision. If it's payer reimbursement and revenue protection - the largest financial lever in most provider organizations - MD Clarity's PayerMonitor is the strongest choice on the market because it was built for that problem rather than retrofitted for it. The platform's purpose-built AI, citation-traceable outputs, integration with underpayment detection and revenue recovery, and transparent published pricing make it the only true payer contract management software on this list.
Every other vendor here is either a general CLM that can store payer contracts as part of a broader portfolio, a healthcare CLM focused on compliance rather than reimbursement, or an enterprise platform with payer features as a vertical solution. Each has legitimate strengths for organizations whose contract problems extend beyond payer agreements - particularly Icertis for Fortune-class enterprises, symplr and Ntracts for compliance-led healthcare operations, and the various enterprise CLMs for legal and procurement-driven contract operations.
The single biggest mistake provider organizations make is buying generic CLM software because it has a "healthcare" page on its website, then discovering months later that storing payer contracts in a general repository didn't actually solve the underpayment problem. Payer contracts deserve payer-specific tools. Ready to see what purpose-built payer contract management looks like? Request a demo from MD Clarity to see how AI-native payer contract management can turn your agreements into recovered revenue.
Take a quick, self-guided demo through a powerful AI-native payer contract management solution:
Get paid in full by bringing clarity to your revenue cycle


.avif)
.png)

